NIV & Significant Outcomes

As a Registered Respiratory Therapist for over 20 years, 17 of those years being in-home care, I have personally set up many severe patients on Non-Invasive Ventilation; and what I see is the amazing positive impact on the patients’ quality of life.
PATIENT IMPACT
Let me tell you about the first woman whom I set up on NIV therapy. She had been struggling with COPD progression for years and had been admitted to the hospital four times in six months. Her quality of life was completely diminished, so much so that when I went to her home, she was winded just answering the door. I went over the use of the machine and then I placed the mask on her face. Within a few short minutes, I could see her work of breathing ease. I let her rest with it on for twenty minutes and then I gently touched her arm to let her know I was going to remove the mask and turn off the machine. The smile on her face was priceless—and something I will never forget. When I called her to follow up on how her NIV therapy was going, she said that she was back to doing many of her daily routines. She could not be more thankful for her machine and the care Frontier Home Medical provided to her.
CARE FROM FRONTIER
Our clinic support specialists always strive to be a point of reference to our referral sources and patients. We work closely with all our providers to offer problem-solving solutions and the best options for patients and their insurance coverage. Insurances have strict guidelines that need to be met in order to cover durable medical equipment and sometimes, that can get confusing. No matter the time of day, we are here to get your patient qualified and set-up. Outcomes are our goal and Non-Invasive Ventilation will help reach that goal.

Written By:
Joselin Lockard, RRT
Frontier Home Medical Sales Representative
Kearney and Grand Island
Wellness from the Ground Up

Just like a home needs a solid foundation, so does our body. Properly fitted shoes not only provide comfort but, most importantly, protection. With therapeutic shoes offered by Frontier Home Medical, your patients will benefit from keeping ulcers from forming and prevent foot strains and calluses.
FOOT CARE FOR DIABETIC PATIENTS
Each year, diabetic patients are eligible for one pair of shoes and three pairs of custom inserts. To qualify for shoes through Medicare, the patient prescription must be signed by an MD or DO, and they must have a face-to-face visit with their provider. The notes must explain the medical need for the shoes and inserts. The provider must certify that the patient has diabetes, and he or she is treating the patient under a comprehensive plan of care.
STATE-OF-THE-ART FIT
After we receive the order, Frontier will contact the patient for a shoe fitting. During our visit, we will measure the patient’s feet, look for any necessary accommodations (such as toe fillers) and scan the patient’s feet with a
3-D camera that creates an exact map around which custom inserts are then molded. These custom inserts can help provide balance and relieve pain in areas like the lower back, knees and neck.
EXPERTISE & CARE
Frontier Home Medical takes pride in providing patients with the best quality and care needed. Please contact one of our certified shoe fitting specialists with any questions regarding our therapeutic shoe line.We are eager to assist you in getting your patients the comfort they deserve!

Written By:
Elsie Hosick
Certified Shoe Fitting Specialist & Customer Service Representative
Supporting Independence

At our formation, the concept of HOME was at the center of what Frontier set out to be. So much so that it was included in our very name—Frontier Home Medical. Home is where we go for comfort, relaxation and contentment. No matter our age, we all strive for and enjoy independence. The importance of being independent is twofold for seniors. First, it is sometimes the only thing seniors may feel they can control as certain aspects of their life change with age. Secondly, maintaining independence promotes a sense of achievement that generates a profound sense of self-worth and well-being for many seniors.
How do we keep people at home?
Unfortunately, there are times when our environment becomes an obstacle or an unsafe place to be. At Frontier Home Medical, we have the equipment and expertise available to help your patients maintain independence and stay in their own homes with little or no help for as long as they desire.
Items as simple as a properly placed grab bar can mean that a person can safely bathe, toilet and even manage areas of their home that might be difficult to maneuver. If a person is unsteady on their feet and at risk for falling, a cane, walker or rollator can make the difference between sitting at home being sedentary—a risk for heart disease and many other ills—and getting out and engaging in other activities. Items such as ramps, porch lifts and stair glides become a vital tool in maintaining safety and independence in a home they may otherwise have to move out of.

Written By:
Anne Seaman
Frontier Home Medical Sales Representative
McCook, North Platte, Cozad
“Hey Doc, Why do I get so many Infections in my Lungs?” Solutions When a Patient Struggles to Breathe
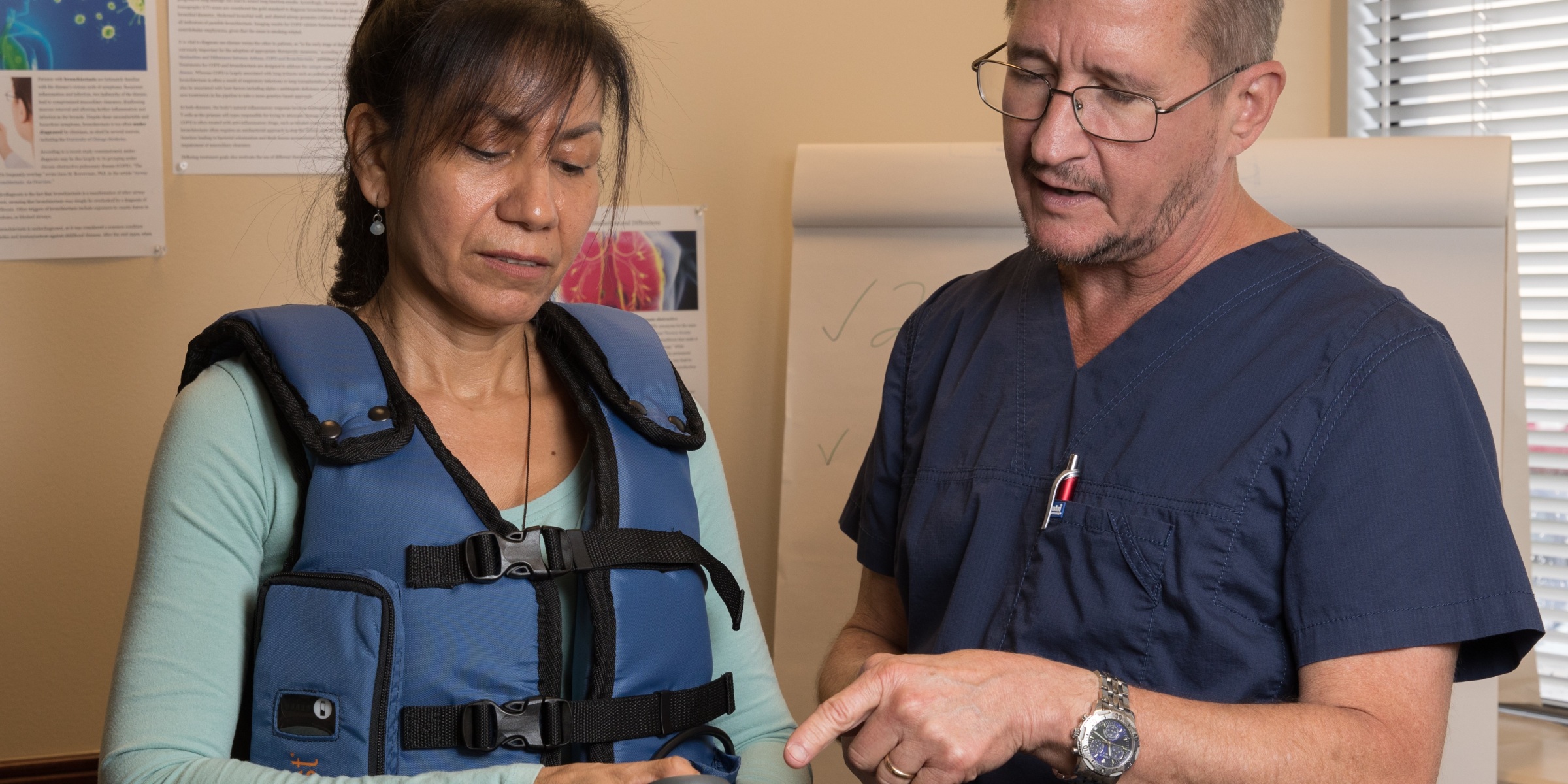
For healthcare providers, it must be frustrating when you feel like you are running out of solutions for a patient who is having issues breathing. Airway clearance is the cornerstone of therapy aimed at minimizing the effects of airway obstruction, infection and inflammation.
THE IMPACT OF HFCWO
AffloVest® is a portable High Frequency Chest Wall Oscillation (HFCWO) vest. It is fully mobile and engineered to mimic anatomically-targeted chest physical therapy. It is an effective airway clearance therapy for improving bronchial drainage by mobilizing secretions.
The AffloVest® has a programmable controller, 9 total setting variations and 3 modes of oscillation treatment (percussion, vibration and drainage) and 3 intensity levels.
The patient simply does two 30-minute sessions per day – all of which can be done in the comfort of home or on the go. Imagine your patient getting the therapy they need while shopping, exercising and even traveling, resulting in consistent therapy compliance. The therapy can be tailored with the 8 anatomically positioned motors to create individual pressure waveforms to target all lobes of the lungs to mobilize those secretions. The AffloVest® comes in 7 different sizes to fit young children and adults.
You can now offer your patient a tool to help break the vicious cycle of inflammation, lung infection and mucus production. The impact that airway clearance has on the patient can include fewer antibiotic prescriptions, fewer hospitalizations and the ability to breathe easier and live a move active, healthy life.
FRONTIER’S EXPERTISE
It has been wonderful to see first-hand the benefits that the AffloVest® can have on patients since we started offering it in 2018. We have set up many patients with vests across the state. It has become another piece of full and complete care of our respiratory patients. We are proud to be considered as the airway clearance specialists in Nebraska. We take a hands-on approach to the care of these individuals who suffer with the simple task of breathing, something that many people take for granted. Patients are always treated with expertise and compassion.
Your Frontier Representatives are happy to demonstrate the AffloVest® and answer questions regarding this therapy and insurance qualifications.

Written By:
Anne Seaman
Frontier Home Medical Sales Representative
Cozad, North Platte, McCook
Kind & Compassionate Incontinence Care: Partnering With Frontier

Loss of bladder and/or bowel control (LOBC) is a sensitive topic for many individuals, and Frontier’s team of certified continence coaches always keeps that in mind. Our kind, caring voices on the other end of the line help develop trust and communication between ourselves and patients. We find that when people are comfortable, they can open up about specific needs, such as needing a heavier absorbency or a product that allows them to leave their homes without worrying about embarrassing accidents.
The Patient Experience
From start to finish, patients discuss incontinence needs with a live person. Beginning with an overview of the incontinent supply program and setting up discreet shipping right to their door, the personal communication continues every month. I, or one of my team members, check in with patients on a monthly basis. We ask if the products they are using are still working properly, if they need additional products and just to touch base. Sometimes that means catching up on what our patients did since we last spoke, including whose grandchildren came to visit, who canned the most apples and whose dog attended church (and didn’t even bark). That’s the most rewarding part for me. I look forward to speaking to our clients—and, I’m told, vice versa; I genuinely love hearing the stories and updates. Our team’s personal touch is just part of our thoughtful and compassionate incontinence program.
The Incontinence Supply Program
Our main goal for working with healthcare professionals is to make the process run smoothly. Within 24-hours of receiving a prescription, we contact your patient and gather the information needed to offer them the best possible products. Then, we send a certification of medical necessity (CMN) to the patient’s provider for signature; this will include specific products, each individually listed. Then the products are packed and shipped, to be repeated as needed each month.
Choosing Frontier to provide incontinence products to your patients is how you can ensure they receive the right products for their needs and are treated with respect. We work with providers across the state to help patients maintain and live their best lives with dignity.

About the Author
Valerie Remmenga is the department manager. She has been with Frontier Home Medical since 2016 as a specialist on Supplemental Nutritional, Sleep Therapy Resupply and Incontinence solutions. If you have questions, contact Valerie and her team at 888.326.3818, M-F, 8 am to 5 pm.
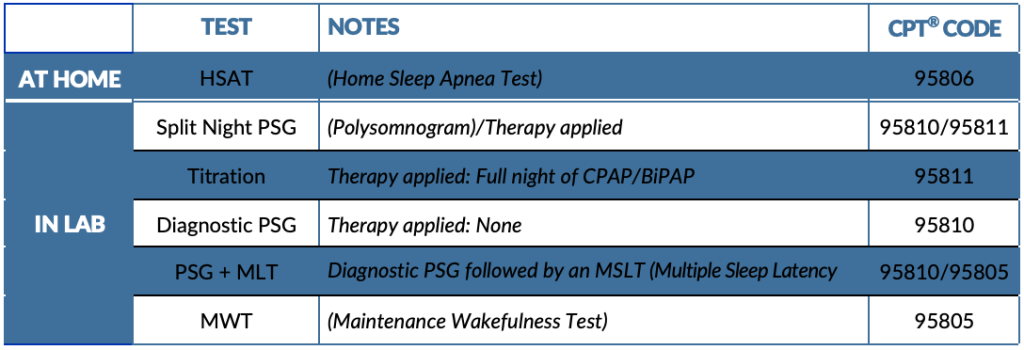
HST vs. PSG

Home sleep testing, or an HST, is a less expensive and more convenient method for the patient who is approved by most insurance companies. The testing equipment simply consists of a chest belt, finger probe and nasal cannula, making it more comfortable and less obtrusive—plus, the patient can complete the test in the comfort of his or her own home. Home sleep testing primarily tests for both obstructive and central sleep apnea. Many insurance companies require a home sleep test before they will approve further testing, like an in-lab study.
PSGs (polysomnograms), also known as in-lab sleep testing, are more thorough studies done with a registered sleep technician on hand. Because the test monitors brain wave activity, movement and heart rhythm, PSGs test for a more comprehensive array of sleep disorders, in addition to sleep apnea.
In-lab testing also allows for more precise results because the sleep tech can use visual observations to record when the patient is actually sleeping. If needed, the patient can be put on PAP therapy during their sleep test, which can show the diagnostic response to pressure treatment in a lab setting.
All tests are scored by a Registered Polysomnographic Technologist (RPSGT) / Registered Respiratory Therapist (RRT), interpreted by a board-certified sleep physician and then sent back to the ordering physician.

Written By:
Levi Jenkins,
RRT, RPSGT
Frontier Diagnostic Sleep Center – Clinical Coordinator
Breath-by-Breath Care

OUR NON-INVASIVE VENTILATION PROGRAM
At Frontier Home Medical, our NIV program is built to be just that – a comprehensive therapy program. We provide equipment and expertise, but we go beyond that. Frontier focuses heavily on educating patients on respiratory impairment, therapy compliance and how home ventilation can improve our patients’ quality of life. Our goal is to hold ourselves to a higher standard of patient care. In doing so, we ensure every effort optimizes therapy quickly, maximizes benefit and lowers hospital readmissions.
We achieve our goal through:
- On-going patient education
- Regularly scheduled follow-up visits with patients
- Weekly compliance checks by experiences respiratory therapists
- 24/7 on-call staff ensuring patients have the necessary support when needed
FIRST IMPRESSIONS
Introducing patients to NIV and their need for home ventilation begins during our initial interaction with the patient and continues with our initial face-to-face visit. At that time, we provide patients with a comprehensive guide to home ventilation therapy. The in-depth content covers specific respiratory disorders, the advantages and goals of using home ventilation therapy, maintenance of supplies, travel tips and compliance requirements. Patients are also provided with a step-by-step device manual with colorful pictures outlining assembly of their equipment, steps taken before starting therapy, stopping therapy and how to respond to alarms.
COMPLIANCE & FOLLOW UP
After the initial set-up is complete, our therapists—in combination with our PAP compliance specialist, monitor patients closely for subjective and objective improvements. We help patients understand that improving their overall well-being starts with consistent usage of their device. As therapists, we know that maximizing compliance starts with maximizing patient comfort. Thus, we make regularly scheduled follow-up visits with patients via telephone or face-to-face, which is a high priority to address any concerns patients may have with therapy settings or equipment-related issues. Our follow-up visits are done routinely—at 24 to 48 hours, seven days, one month, two months, three months post set-up, every 90 days and as needed thereafter, so as the ordering provider, you can rest assured knowing that your patient is adequately cared for. Upon completion of each 90-day visit, physicians and practitioners are provided with assessment notes and compliance reports on their patients.
BIPAP VS. NIV
To any provider considering BiPAP (or BiLevel) therapy for home use, it is essential to know that a more reliable therapy option for your patient with chronic hypercapnia and/or respiratory failure is available. Standard BiPAP devices utilize fixed pressures to deliver a target tidal volume; however, the actual volume delivered can often be very inconsistent and is not guaranteed, potentially resulting in an exacerbation, hospitalization or both. This especially becomes true as patients’ conditions change over time. On the other hand, NIV guarantees either a set tidal volume or minute ventilation is delivered to the patient by utilizing a “pressure range” instead, ensuring that as patients’ ventilation needs change, they will continue to be met—guaranteed.
DEDICATION TO CARE
Having worked in a variety of healthcare settings over the past decade, I believe that education is vital to providing the best care possible and ensuring the best quality of life. This has never been more true to me as of last year when my father underwent an emergent mitral valve repair that was close to being fatal. During his recovery, I witnessed firsthand the impact that in-depth patient education, as well as proper therapy management and support, can have on patient outcomes. My father is doing great and continues to thrive thanks to all of his providers who took the time to educate and support him to this day. Educating and supporting have become the foundation of our program here at Frontier. As providers, we make recommendations to our patients every day who trust us to ensure their well-being and I assume their trust in me as a personal responsibility. That’s why developing strong, trusting relationships is the foundation of everything I do, both professionally and personally. When it comes to NIV and the impact it can have on patients’ lives, such as being able to walk up a full flight of stairs for the first time in 7 years or being able to garden again without getting short of breath, my promise to every patient we care for or provider we work with is your support and clinical expertise is always just a phone call away.

Written By:
Brandon Baker, BS, RRT
Brandon is Frontier’s Respiratory Disease Manager specializing primarily in Non-Invasive Ventilation. He previously worked in EMS as a paramedic for 10 years, as an adjunct EMS instructor for 2 years and a hospital respiratory therapist.
Qualifying Medicare Patients for Therapeutic Shoes


For someone diagnosed with diabetes mellitus, Medicare may cover the cost of therapeutic shoes and custom inserts; however, specific criteria must be met in a face-to-face exam. First, only a Medical Doctor (MD) or a Doctor of Osteopathy (DO) can order diabetic-friendly footwear and inserts. If the face-to-face is completed by a Podiatrist, Physician’s Assistant (PA-C) or Nurse Practitioner (APRN/NP), then there must be a physician who agrees with the foot exam and plan for shoes/inserts.
The physician must certify that the patient has diabetes and is under a comprehensive plan of care for his/her diabetes. It must also document that the patient suffers from one or more of the following conditions (the more specific the better):
- Amputation of the foot or part of the foot
- History of previous foot ulceration of either foot
- History of pre-ulcerative calluses of either foot
- Peripheral neuropathy with evidence of callus formation of either foot
- Foot deformity of either foot
- Poor circulation of either foot
Medicare will cover the cost of the therapeutic shoes and inserts if all of the criteria is met. They will cover one new pair of therapeutic shoes per calendar year, along with three pairs of custom inserts
HCPCS To Know
A5500 Therapeutic Shoes
A5514 Insert (Camera-Tech Molded)
A5513 Insert (Foot-Contact Molded)
A5512 Insert (Heat Moldable)

Written by:
Joselin Lockard, RRT
Frontier Home Medical Sales Representative
(Kearney, Grand Island, Lincoln)
IF IT WERE YOUR PARENT… WHY CHOOSE FRONTIER HOME MEDICAL FOR OXYGEN NEEDS

Patients have many questions and concerns when choosing a home care company to provide them with oxygen.
WILL THE COMPANY MY PATIENTS CHOOSE KNOW THE EQUIPMENT THAT IS BEST FOR THEM?
At Frontier Home Medical, we know that each oxygen device has its own benefits and features. Understanding the patient’s prescription, lifestyle and usage needs will help us determine just the right oxygen device. We call it the Best Match Protocol.
WILL THEY PROVIDE ON CALL SERVICE?
We offer a 24/7 After Hours Emergency Line. In addition, trained on-call staff is available for oxygen setups.
WILL THEY EDUCATE MY PATIENTS ON THEIR EQUIPMENT AND HOW THEIR EQUIPMENT HELPS WITH THEIR DISEASE?
At Frontier, patients receive a consultation with trained Patient Care Technicians during equipment set up and are given simple, easy-to-understand educational
materials to read and refer to. We also have on-staff Respiratory Therapists to answer any questions your patients may have.
WILL THEY WORK WITH ME AND MY PATIENT’S INSURANCE COMPANY TO SEE THAT EVERYTHING IS DONE TO QUALIFY SO MY PATIENTS CAN TAKE FULL ADVANTAGE OF THEIR BENEFITS?
Yes, the billing experts at Frontier Home Medical work closely with providers and insurance companies. This is such an essential piece of the process, to know upfront what is needed to qualify a patient for equipment and also communicate what, if any, financial responsibility may be.
WHAT IS THE DIFFERENCE BETWEEN CONTINUOUS FLOW AND PULSE FLOW?
Continuous flow gives a steady stream of oxygen; pulse flow is based on breath rates. For patients who do not require a heavier concentration of oxygen, the convenience of pulse flow oxygen may be something to consider for your patient’s needs.
WILL MY PATIENTS BE ABLE TO TRAVEL?
Traveling with oxygen by car or other means of transportation may seem intimidating. However, with a little planning, it can be easily, and safely, done. At Frontier, we can offer patients several options that make traveling easier, such as Portable Oxygen Concentrators and small tanks with conserving devices. It’s always a good idea for your patients to have a letter and copy of their prescription with them during travel.
WHY IS FRONTIER THE BEST CHOICE?
Patients truly are in good hands at Frontier Home Medical. We have the equipment and clinical expertise to find the right product for each person’s needs. Patients have access to on-staff Respiratory Therapists. They get consultation with trained Patient Care Technicians during set up. We are experts in insurance coverage. When it comes to oxygen therapy, we have it covered!
Written by: Anne Seaman – Frontier Home Medical Sales Representative (Cozad, McCook, North Platte)
Pressure Ulcers Guidelines

Risk assessment and prevention of pressure ulcers:
a clinical practice guideline from the American College of Physicians
Authors: Amir Qaseem, Tanveer P Mir, Melissa Starkey, Thomas D Denberg
Publisher: Clinical Guidelines Committee of the American College of Physicians
Abstract: The American College of Physicians (ACP) developed this guideline to present the evidence and provide clinical recommendations based on the comparative effectiveness of risk assessment scales and preventive interventions for pressure ulcers.

Methods: This guideline is based on published literature on this topic that was identified by using MEDLINE (1946 through February 2014), CINAHL (1998 through February 2014), the Cochrane Library, clinical trials registries, and reference lists. Searches were limited to English-language publications. The outcomes evaluated for this guideline include pressure ulcer incidence and severity, resource use, diagnostic accuracy, measures of risk, and harms. This guideline grades the quality of evidence and strength of recommendations by using ACP’s clinical practice guidelines grading system. The target audience for this guideline includes all clinicians, and the target patient population is patients at risk for pressure ulcers.
Full text: https://pubmed.ncbi.nlm.nih.gov/25732278/